Why Do I Keep Getting Strep Throat? Recurring strep throat is a frustrating and painful experience that leaves many people searching desperately for answers.
Strep throat is caused by Group A Streptococcus bacteria, and some individuals are simply more vulnerable to repeated infections than others.
Common reasons include a weakened immune system, frequent close contact with infected individuals, or being a silent carrier of the bacteria without realizing it.
Children are particularly susceptible due to their developing immune systems and close school environments.
Incomplete antibiotic treatment can also allow bacteria to survive and return. Chronic cases may ultimately require a tonsillectomy to permanently resolve the problem.
Table of Contents
Quick Table
| Cause | Details |
|---|---|
| Group A Streptococcus | The specific bacteria responsible for all strep throat infections |
| Weakened Immune System | Low immunity makes it harder to fight off recurring bacterial infections |
| Silent Carrier | Some people carry the bacteria without symptoms and reinfect themselves |
| Close Contact | Living or working near infected individuals increases exposure significantly |
| Incomplete Antibiotics | Not finishing prescribed antibiotics allows bacteria to survive and return |
| School Environments | Children face higher risk due to crowded classrooms and shared surfaces |
| Household Transmission | Family members passing bacteria back and forth within the same home |
| Tonsil Size | Larger tonsils trap more bacteria, increasing frequency of infections |
| Poor Hand Hygiene | Touching face and mouth with unwashed hands spreads bacteria easily |
| Sharing Personal Items | Sharing utensils, drinks, or towels transfers bacteria between individuals |
| Stress and Fatigue | Chronic stress weakens immune response and increases infection vulnerability |
| Tonsillectomy | Surgical removal of tonsils recommended for chronic recurring strep cases |
| When to See a Doctor | Four or more strep infections per year warrants immediate medical evaluation |
Why Do I Keep Getting Strep Throat?
I remember sitting in an urgent care waiting room for the third time in six months, staring at the ceiling, thinking — what is wrong with me?
Every time I thought I was finally better, the fever would creep back, the swallowing would become agony, and I’d be back on antibiotics.
The doctor would do a rapid strep test, it would come back positive, and she’d hand me a prescription for amoxicillin like clockwork. I’d finish the course, feel great for a few weeks, and then… bam. Round four.
If you’re reading this, you’re probably living the same miserable loop. Let me save you some time — and honestly, some pain — by walking you through what I learned after way too many strep infections.
First, Why Does Strep Keep Coming Back?
The frustrating truth is that recurring strep throat isn’t just bad luck. There are usually very specific reasons it keeps happening, and once you understand them, the solution becomes a lot clearer.
You Might Not Be Fully Clearing the Infection
This one caught me off guard. I’d feel better around day four or five and start skipping doses here and there. Felt fine, right? Wrong.
Group A Streptococcus (that’s the bacteria behind strep throat) is stubborn.
If you don’t finish the full antibiotic course — usually 10 days of amoxicillin — you’re leaving behind a small population of bacteria that can regroup and come back stronger.
I got lectured about this by a doctor who was clearly tired of seeing me. She made me set phone alarms for every dose. Annoying? Yes. Effective? Also yes.
Someone in Your Household Is a Carrier
This is the one people don’t think about — and it blew my mind when I found out. Some people carry strep bacteria in their throat without ever getting sick themselves.
They feel totally fine but are quietly re-infecting everyone around them.
I kept getting strep while my roommate never complained of a sore throat once. Turns out, he was a strep carrier. Classic.
If you live with family, a partner, or roommates and keep getting reinfected, it’s absolutely worth asking your doctor about testing everyone in the house.
This is probably the most overlooked reason for recurring strep.
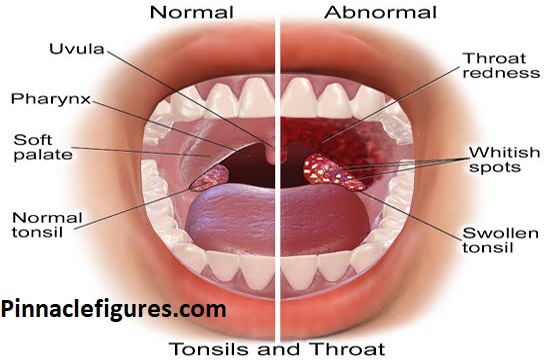
Your Tonsils Might Be the Problem
Tonsils are great at trapping bacteria — that’s kind of their job. But if they’re chronically inflamed or have deep pockets (called crypts), bacteria can hide in there and avoid antibiotics entirely.
Your throat looks fine on the surface, but the infection is just lurking.
If you’re getting strep five or more times a year, your doctor might start talking about a tonsillectomy. I know that sounds extreme, but for a lot of people — especially adults — it’s genuinely life-changing.
No more recurring infections.
You’re Re-Exposing Yourself (And You Don’t Know It)
Here’s something I never would have thought of on my own: your toothbrush.
Strep bacteria can live on your toothbrush.
So you finish your antibiotics, brush your teeth with the same brush you used while sick, and reintroduce the bacteria right back into your throat.
After my fourth infection, I started replacing my toothbrush (or sanitizing it) the moment I started antibiotics and again after I finished. Small change, made a real difference.
Same goes for things like water bottles, lip balm, pillowcases, and anything else that regularly touches your mouth. Wash them. Seriously.
Stress and a Weakened Immune System
My worst streak of strep infections happened during the most stressful period of my life — back-to-back work deadlines, terrible sleep, surviving mostly on coffee and stress.
My immune system was basically waving a white flag.
Chronic stress tanks your immune response. Lack of sleep does the same.
When your body is running on empty, even a brief exposure to strep bacteria can turn into a full infection, because your immune system doesn’t have the energy to fight it off before it takes hold.
I’m not saying stress management is a cure, but it’s genuinely part of the picture.
What You Can Actually Do About It
Okay, enough diagnosing the problem. Here’s the practical stuff.
Talk to Your Doctor About the Pattern
Don’t just go in asking for antibiotics. Go in and say: “I’ve had strep X times this year, and I want to understand why.” That framing opens a completely different conversation.
Ask specifically about:
- Household carrier testing
- Whether a throat culture (not just a rapid test) has been done — rapid tests miss about 10-30% of infections
- Whether your tonsils are contributing to the problem
- Whether a referral to an ENT (ear, nose, and throat specialist) makes sense
Always Finish Your Antibiotics
I know I already said this, but it bears repeating because I ignored it myself for years. The full 10-day course exists for a reason. Even if you feel 100% on day six, those last four days matter.
Set phone alarms. Put the pill bottle next to your coffee maker. Do whatever you need to actually finish the course.
Replace Your Toothbrush
This is free advice that nobody gives you in the exam room. The moment you test positive for strep, get a new toothbrush or UV-sanitize your electric brush head.
Replace it again when you finish antibiotics. If you use a reusable water bottle, wash it thoroughly during and after illness.
Ask Your Doctor About Household Testing
If you live with other people and keep getting reinfected, bring it up directly.
A simple throat swab can identify carriers. Carriers might need a short course of antibiotics to clear the bacteria, even though they have no symptoms.
This step alone stopped my recurring infections.
Consider an ENT Consultation
If you’ve had three or more documented strep infections in a year (or five in two years), most guidelines suggest at least talking to an ENT about your options.
Tonsillectomy isn’t the automatic answer, but it’s worth the conversation.
Adult tonsillectomies are rougher to recover from than childhood ones, I won’t lie. But people who’ve had chronic strep for years almost universally say it was worth it.
Mistakes I Made (So You Don’t Have To)
Stopping antibiotics early. Did it multiple times. Regretted it every time.
Not replacing my toothbrush. Didn’t even occur to me until a nurse mentioned it offhand.
Assuming it was a new exposure every time. Sometimes it was literally the same infection, incompletely treated.
Not pushing for a throat culture. Rapid strep tests are convenient but not perfect. If your test comes back negative but you feel exactly like you do when you have strep, ask for a throat culture to be sent to a lab. It takes a day or two but is more accurate.
Treating the symptoms without asking why. I took antibiotics six times before I finally had a real conversation with my doctor about the root cause. Don’t wait that long.
When Should You Actually Worry?
Most recurring strep is annoying and miserable, but not dangerous. However, there are a few situations where you should be seen quickly:
- You have a high fever (above 103°F / 39.4°C) that isn’t coming down with medication
- You have trouble breathing or swallowing
- You notice swelling on one side of your throat that looks asymmetrical — this can indicate a peritonsillar abscess, which needs immediate treatment
- Your symptoms don’t improve at all after two to three days on antibiotics
FAQs
How many strep infections per year is considered chronic?
Most doctors consider four or more confirmed strep throat infections within a single year as chronic recurring strep. At this point, a referral to an ear, nose, and throat specialist is strongly recommended to explore longer term solutions.
Can you be a strep carrier without knowing it?
Yes. Some individuals carry Group A Streptococcus bacteria in their throat without ever developing symptoms themselves. However, they can still unknowingly transmit the infection to others around them through close contact and shared surfaces.
Will a tonsillectomy permanently stop strep throat?
A tonsillectomy significantly reduces the frequency and severity of strep infections for most patients. While it does not guarantee complete elimination since bacteria can still infect throat tissue, the majority of patients experience dramatic long term improvement.
Can stress really cause recurring strep throat?
Stress does not directly cause strep throat but chronically elevated stress hormones suppress immune function, making your body considerably less capable of fighting off bacterial infections like Group A Streptococcus when exposed.
Should children with recurring strep have their tonsils removed?
Pediatric guidelines generally recommend considering tonsillectomy for children experiencing seven or more infections in one year, five per year over two consecutive years, or three per year over three consecutive years.
Conclusion
Recurring strep throat is more than just a nuisance — it is a genuine medical concern that deserves proper attention, thorough investigation, and a thoughtful long term management plan.
For those who find themselves battling this painful infection multiple times a year, understanding the underlying reasons is the critical first step toward finally breaking the exhausting cycle of illness, antibiotics, and temporary recovery.
The causes of recurring strep are varied and often interconnected.
A weakened immune system, silent bacterial carriers within the household, incomplete antibiotic courses, and environmental exposure all play significant roles in why some individuals simply cannot seem to shake this stubborn infection.
Identifying and addressing each contributing factor gives the body its best possible chance at sustained recovery.
Good hygiene habits, completing every prescribed antibiotic course, and minimizing close contact during active infections are practical steps every patient can take immediately.
However, when these measures prove insufficient and infections continue piling up, medical intervention becomes not just reasonable but necessary.
A tonsillectomy, while a significant decision, has provided lasting relief for countless patients who once felt trapped in an endless cycle of strep infections.
Consulting an ear, nose, and throat specialist opens the door to personalized solutions tailored specifically to your medical history and needs.
