Why Do My Ankles Swell? Ankle swelling — medically known as peripheral edema — refers to an abnormal buildup of fluid in the tissues surrounding the ankle joint and lower leg.
It is one of the most common physical complaints seen by primary care physicians, emergency departments, and orthopedic specialists alike.
The swelling may affect one ankle (unilateral) or both (bilateral), and it may appear suddenly or develop gradually over days, weeks, or even months.
At its most basic level, ankle swelling occurs when fluid leaks out of tiny blood vessels (capillaries) into surrounding soft tissue.
This can happen for many reasons: increased pressure within vessels, reduced protein in the blood, inflammation, injury, or obstruction of the lymphatic system.
Table of Contents
Quick Table
| Cause | One or Both Ankles? | Pain Level | Onset | Key Associated Symptoms | Urgency |
|---|---|---|---|---|---|
| Prolonged sitting/standing | Both | None to mild | Gradual | Resolves with rest & elevation | Low — monitor at home |
| Ankle sprain | One | Moderate to severe | Sudden | Bruising, difficulty walking | Low to moderate — see doctor if severe |
| Venous insufficiency | Both | Mild aching | Gradual, chronic | Varicose veins, skin discoloration, worse at end of day | Low — routine appointment |
| Heart failure | Both | None | Gradual | Shortness of breath, fatigue, rapid weight gain | High — see doctor promptly |
| Deep vein thrombosis (DVT) | One | Moderate to severe | Sudden | Warmth, redness, leg pain | Emergency — seek care immediately |
| Kidney disease | Both | None | Gradual | Foamy urine, puffy eyes, fatigue | High — see doctor promptly |
| Liver disease (cirrhosis) | Both | None to mild | Gradual | Jaundice, abdominal swelling, easy bruising | High — see doctor promptly |
| Pregnancy | Both | None to mild | Gradual | Worse in third trimester; if sudden + headache → emergency | Low (mild) / Emergency (severe) |
| Medication side effect | Both | None | Gradual | Begins after starting new medication | Moderate — consult your doctor |
| Lymphedema | One or both | None to mild | Gradual, chronic | Non-pitting, does not improve with elevation | Moderate — routine appointment |
| Hypothyroidism | Both | None | Gradual | Fatigue, weight gain, cold intolerance, non-pitting | Moderate — routine appointment |
| Cellulitis (infection) | One | Moderate to severe | Rapid | Redness, warmth, fever, spreading skin changes | High — see doctor within 24 hrs |
| Gout / Arthritis | One (usually) | Severe | Sudden | Red, hot, extremely tender joint | High — see doctor promptly |
| Fracture / Trauma | One | Severe | Sudden | Bruising, deformity, inability to bear weight | Emergency — seek care immediately |
Why Do My Ankles Swell?
Swollen ankles, known as edema, happen when excess fluid builds up in tissues. Common causes include long periods of standing or sitting, hot weather, or high salt intake.
Medical conditions like heart failure, kidney disease, or venous insufficiency can also lead to swelling. Hormonal changes, pregnancy, or certain medications may contribute as well.
If swelling is sudden, painful, or persistent, it could signal a serious issue like a blood clot. Elevating your legs, reducing salt, and staying active can help, but ongoing symptoms should be evaluated by a doctor.
14 Common Causes of Ankle Swelling
Prolonged Standing or Sitting
When you stand or sit for long periods without movement — during a long flight, a desk job, or a lengthy car ride — gravity pulls blood and fluids downward into the lower extremities.
The venous system struggles to return blood upward efficiently, and fluid leaks into surrounding tissue. This is one of the most common and benign causes of ankle swelling. It typically resolves with elevation and movement.
Sprained Ankle
An ankle sprain involves overstretching or tearing of the ligaments that stabilize the joint. It usually occurs during activities that twist or roll the ankle — stepping off a curb, landing awkwardly from a jump, or slipping on uneven ground.
The body’s inflammatory response floods the area with fluid, causing rapid and often dramatic swelling, bruising, and pain. Sprains are graded from Grade I (mild stretching) to Grade III (complete ligament tear).
Venous Insufficiency
Chronic venous insufficiency (CVI) occurs when the one-way valves inside the leg veins become damaged or weakened, allowing blood to pool in the lower legs rather than returning to the heart.
Over time, this increased venous pressure forces fluid into surrounding tissues. Symptoms include bilateral ankle and leg swelling that is typically worse at the end of the day and after prolonged standing.
Varicose veins, skin discoloration (a brownish tinge called hyperpigmentation), and skin thickening (lipodermatosclerosis) are common accompanying signs.
Heart Failure
When the heart cannot pump blood effectively, fluid backs up in the body. Right-sided heart failure, in particular, leads to fluid accumulation in the venous circulation, resulting in bilateral ankle and leg swelling (pedal edema).
The swelling is typically pitting and worse in the evening. It is often accompanied by shortness of breath, fatigue, and reduced exercise tolerance.
Heart failure is one of the most important and serious causes of bilateral ankle swelling and requires prompt medical evaluation.
Deep Vein Thrombosis (DVT)
A deep vein thrombosis is a blood clot that forms in one of the deep veins of the leg, most commonly in the calf or thigh. It causes sudden, often unilateral swelling, pain, warmth, and redness in the affected leg.
DVT is a medical emergency because the clot can dislodge and travel to the lungs, causing a potentially life-threatening pulmonary embolism (PE).
Risk factors include prolonged immobility, recent surgery, pregnancy, cancer, and certain blood-clotting disorders.
Kidney Disease or Nephrotic Syndrome
The kidneys play a vital role in regulating fluid balance. When kidneys are damaged or fail, they may lose their ability to filter excess fluid and waste, or they may leak large amounts of protein (albumin) into the urine.
Low albumin in the blood reduces the osmotic pressure that keeps fluid inside blood vessels, causing fluid to leak into tissues — a condition called nephrotic syndrome.
Ankle and leg swelling is a hallmark symptom, along with foamy urine (proteinuria), fatigue, and puffy eyes (periorbital edema).
Liver Disease (Cirrhosis)
Advanced liver disease, particularly cirrhosis, reduces the liver’s ability to produce albumin, the main protein in the blood.
As with kidney disease, low albumin allows fluid to escape into tissues. Liver disease also increases pressure in the portal vein (portal hypertension), contributing to fluid accumulation in the abdominal cavity (ascites) and lower extremities.
Ankle swelling in the context of liver disease may be accompanied by jaundice (yellowing of the skin and eyes), abdominal distension, easy bruising, and fatigue.
Pregnancy
Ankle and leg swelling is extremely common during pregnancy, especially in the third trimester.
The growing uterus puts pressure on the inferior vena cava (the large vein that returns blood from the lower body to the heart), slowing venous return and causing fluid to accumulate in the lower extremities.
Hormonal changes also promote fluid retention.
While mild, symmetrical swelling is normal in pregnancy, sudden or severe swelling — especially in one leg — or swelling accompanied by headache, visual changes, and high blood pressure may indicate preeclampsia, a serious pregnancy complication.
Medications
Many commonly prescribed medications can cause ankle swelling as a side effect. These include:
- Calcium channel blockers (e.g., amlodipine, nifedipine) — widely used for hypertension and heart disease
- NSAIDs (e.g., ibuprofen, naproxen) — cause sodium and water retention
- Corticosteroids (e.g., prednisone) — promote fluid retention
- Thiazolidinediones (e.g., pioglitazone, rosiglitazone) — diabetes medications known to cause edema
- Certain antidepressants and mood stabilizers
- Hormone therapy and oral contraceptives — estrogen-containing medications promote fluid retention
If you suspect a medication is causing your ankle swelling, consult your doctor before stopping or changing your medication.
Lymphedema
Lymphedema results from damage or obstruction to the lymphatic system — the network of vessels and nodes that drains excess fluid from tissues and returns it to the bloodstream.
When lymphatic drainage is impaired, protein-rich fluid accumulates in the limb, causing chronic, often non-pitting swelling.
Primary lymphedema is caused by developmental abnormalities of the lymphatic system.
Secondary lymphedema is far more common and may result from cancer treatment (surgery, radiation), infection, or injury.
The swelling is typically asymmetric and does not improve significantly with elevation alone.

Hypothyroidism (Myxedema)
An underactive thyroid gland produces insufficient thyroid hormone, which can cause a distinctive type of non-pitting edema called myxedema.
Unlike typical fluid edema, myxedema involves the accumulation of glycosaminoglycans in the skin and subcutaneous tissue.
Ankle and lower leg swelling in hypothyroidism is non-pitting, meaning that pressing on the skin does not leave an indentation.
It may be accompanied by fatigue, weight gain, cold intolerance, constipation, dry skin, and slowed heart rate.
Infection or Cellulitis
Bacterial infection of the skin and underlying soft tissue — cellulitis — typically causes localized swelling, redness, warmth, and pain in the affected area.
It most commonly affects the lower legs and can enter through breaks in the skin such as cuts, insect bites, fungal infections, or skin conditions like eczema.
Cellulitis can spread rapidly and may cause systemic symptoms such as fever, chills, and malaise if bacteria enter the bloodstream (sepsis). It requires antibiotic treatment.
Gout or Arthritis
Gout is a form of inflammatory arthritis caused by the accumulation of uric acid crystals in joint spaces.
It most commonly affects the big toe but can also affect the ankle, causing sudden, intense swelling, redness, warmth, and excruciating pain — often waking sufferers from sleep.
Other forms of arthritis, including rheumatoid arthritis and osteoarthritis, can also cause ankle joint swelling, though typically in a more chronic and less acute pattern.
Reactive arthritis (following a bacterial infection) can also cause ankle swelling as part of a broader inflammatory response.
Trauma or Fracture
Any significant injury to the ankle — including fractures, dislocations, or severe contusions — will trigger an immediate and intense inflammatory response with pronounced swelling.
Ankle fractures can range from simple hairline cracks to complex breaks involving multiple bones.
A fracture should be suspected if the swelling follows significant trauma, if there is deformity, if the pain is severe and weight-bearing is impossible, or if there is point tenderness over a bone.
An X-ray is typically necessary to confirm.
Serious vs. Benign How to Tell the Difference
Not all swollen ankles are equal. The distinction between a minor inconvenience and a medical emergency often lies in a combination of the onset, pattern, and accompanying symptoms.
Likely Benign:
- Swelling that develops gradually after prolonged sitting or standing
- Bilateral (both ankles), symmetric swelling that is mild and resolves with rest and elevation
- Swelling associated with hot weather or a salty meal
- Mild swelling in late pregnancy with no other concerning symptoms
- Minor swelling after a known, mild ankle sprain
Potentially Serious — Seek Prompt Medical Attention:
- Sudden swelling in one leg, especially with pain, warmth, or redness (possible DVT)
- Swelling accompanied by shortness of breath, chest pain, or coughing up blood (possible pulmonary embolism or heart failure)
- Rapidly spreading redness, warmth, and fever (possible cellulitis or sepsis)
- Swelling in a pregnant woman with headache, blurred vision, or high blood pressure (possible preeclampsia)
- New swelling with no obvious cause in a person with heart, kidney, or liver disease
- Swelling with significant skin breakdown, ulceration, or discharge
Emergency — Call Emergency Services Immediately:
- Sudden severe shortness of breath with ankle swelling
- Chest pain or pressure with swelling
- Confusion or loss of consciousness with swelling
- Symptoms suggesting a pulmonary embolism (sudden shortness of breath, rapid heart rate, coughing blood)

Associated Symptoms to Watch For
Ankle swelling rarely occurs in a vacuum. The symptoms that accompany it are critical clues to its cause. Pay close attention to:
Cardiovascular and pulmonary symptoms:
- Shortness of breath (especially when lying flat — orthopnea)
- Waking at night breathless (paroxysmal nocturnal dyspnea)
- Rapid or irregular heartbeat
- Chest pain or tightness
- Persistent cough (sometimes with pink, frothy sputum in heart failure)
- Reduced tolerance for exercise
Skin changes:
- Redness, warmth, and tenderness over the swollen area (infection or DVT)
- Skin discoloration — brownish staining (venous insufficiency) or yellowing (liver disease)
- Skin hardening or thickening (chronic venous insufficiency, lymphedema)
- Open sores or ulcers on the lower leg or ankle
- Shiny, taut, stretched skin
Systemic symptoms:
- Fever and chills (infection, DVT, sepsis)
- Unexplained weight gain over days (fluid retention from heart, kidney, or liver disease)
- Fatigue and general malaise
- Decreased urine output or dark urine (kidney disease)
- Foamy urine (protein in urine, suggesting kidney disease)
- Abdominal swelling or pain (liver disease, heart failure)
Musculoskeletal symptoms:
- Pain with movement or weight-bearing (fracture, sprain, gout)
- Joint stiffness (arthritis)
- Bruising (trauma, fracture)
- Deformity of the joint
Neurological symptoms:
- Numbness or tingling in the foot or toes (nerve compression, diabetes)
- Weakness in the foot or leg
Who Is Most at Risk?
While ankle swelling can affect anyone, certain populations are significantly more vulnerable:
Older adults: Aging is associated with reduced venous valve competence, decreased cardiac efficiency, lower serum albumin, reduced physical activity, and greater medication use — all of which increase the risk of ankle edema.
Pregnant women: The physiological changes of pregnancy — including increased blood volume, hormonal shifts, and mechanical compression — make ankle swelling nearly universal by the third trimester.
People with chronic diseases: Those with heart failure, chronic kidney disease, liver cirrhosis, diabetes, or hypothyroidism are at much higher risk of developing edema as a complication of their underlying condition.
Sedentary individuals: People with desk jobs, those who travel frequently by plane or car, or those who are bedridden after illness or surgery are at increased risk of dependent edema and DVT.
Obese individuals: Excess body weight increases venous pressure in the lower extremities, impairs lymphatic drainage, and is associated with many conditions (heart disease, diabetes, venous insufficiency) that cause swelling.
People on certain medications: As described above, users of calcium channel blockers, corticosteroids, NSAIDs, and other medications are at higher risk of drug-induced edema.
Cancer patients: Cancer and its treatments (particularly lymph node removal and radiation) can cause lymphedema. Some cancers also cause venous obstruction.
Athletes and those with physically demanding jobs: Repetitive stress, ankle sprains, and overuse injuries are more common in these groups.
How Doctors Diagnose Ankle Swelling
Diagnosing the cause of ankle swelling requires a systematic approach. Your doctor will typically begin with a thorough history and physical examination and then order targeted tests based on clinical suspicion.
History and Physical Examination: The doctor will ask about the onset, duration, and progression of swelling; whether it affects one or both ankles; whether it is worse at certain times of day; associated symptoms; medical history; medication use; recent travel or immobility; and family history of cardiac or vascular disease.
On examination, the doctor will assess whether the swelling is pitting or non-pitting, measure the circumference of both legs for comparison, inspect the skin for changes, check pulses and capillary refill, auscultate the heart and lungs, palpate the abdomen, and look for tenderness along the course of deep veins.
Blood Tests:
- Complete blood count (CBC) — to assess for infection or anemia
- Comprehensive metabolic panel (CMP) — to evaluate kidney and liver function, and serum albumin
- B-type natriuretic peptide (BNP or NT-proBNP) — elevated in heart failure
- D-dimer — elevated in DVT and pulmonary embolism (used as a screening tool)
- Thyroid function tests (TSH, free T4) — to rule out hypothyroidism
- Uric acid — elevated in gout
Urine Tests:
- Urinalysis — to check for protein, blood, and signs of infection
- 24-hour urine protein — to quantify proteinuria (kidney disease)
Imaging:
- Duplex ultrasound — the gold standard for diagnosing DVT; uses sound waves to visualize blood flow and detect clots in the deep veins
- Echocardiogram (Echo) — ultrasound of the heart to assess cardiac function and diagnose heart failure
- X-ray — to rule out fractures or dislocations
- CT or MRI — used when DVT, venous compression, or complex pathology is suspected
- Lymphoscintigraphy — a nuclear medicine scan used to diagnose lymphedema
Specialized Tests:
- Ankle-brachial index (ABI) — compares blood pressure in the ankle to the arm to assess arterial circulation
- Venous duplex ultrasound — to evaluate venous insufficiency
- Echocardiogram with Doppler — for detailed cardiac assessment
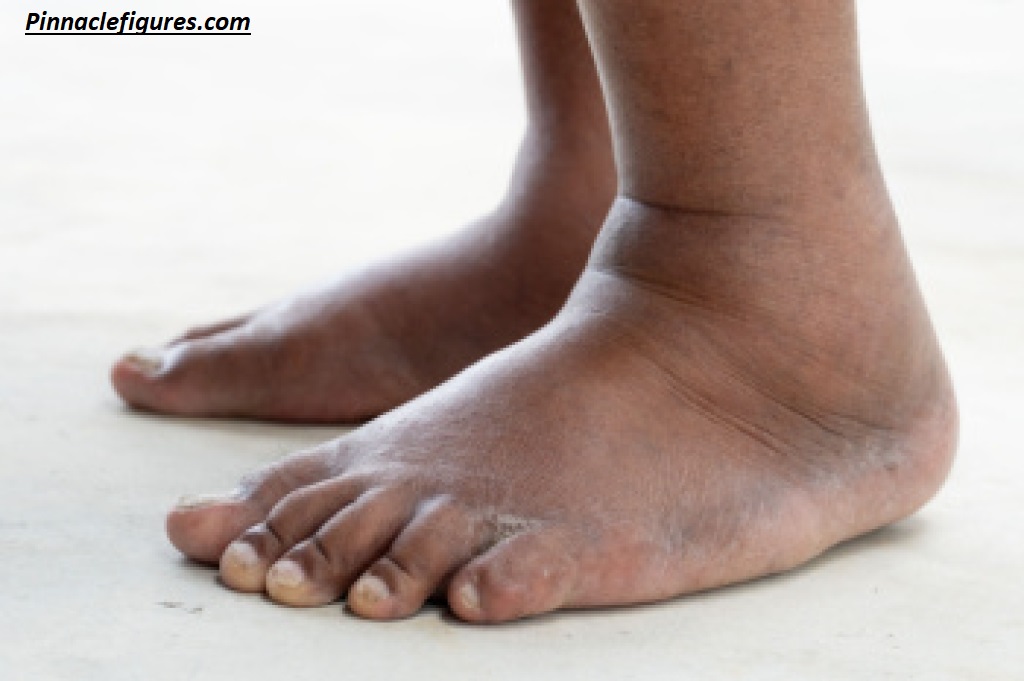
Treatment Options & Home Remedies
Treatment depends entirely on the underlying cause. Addressing the root cause is the most important step. However, several strategies can provide symptomatic relief and reduce swelling regardless of cause.
Medical Treatments
For Heart Failure: Diuretic medications (e.g., furosemide, spironolactone) are the cornerstone of treatment, removing excess fluid from the body through the kidneys.
ACE inhibitors, beta-blockers, and other cardiac medications address the underlying heart dysfunction.
For DVT: Anticoagulant therapy (blood thinners) — typically low-molecular-weight heparin, rivaroxaban, apixaban, or warfarin — is used to prevent clot extension and reduce the risk of pulmonary embolism. Duration of treatment depends on the clinical context.
For Venous Insufficiency: Compression therapy (stockings), leg elevation, and in some cases procedures to address varicose veins (sclerotherapy, laser ablation, surgical stripping) are used.
For Lymphedema: Complete decongestive therapy (CDT) is the gold standard, combining manual lymphatic drainage massage, multilayer compression bandaging, exercises, and skincare. Maintenance compression garments are worn long-term.
For Cellulitis: Oral or intravenous antibiotics, depending on severity.
For Gout: Colchicine, NSAIDs, or corticosteroids for acute attacks; urate-lowering therapy (allopurinol, febuxostat) for prevention.
For Medication-Induced Edema: Reducing the dose, switching to an alternative medication, or adding a diuretic under medical supervision.
For Kidney or Liver Disease: Disease-specific management plus diuretics for symptomatic control.
Home Remedies and Self-Care
RICE Protocol (for acute sprains and injuries):
- Rest — avoid putting weight on the ankle
- Ice — apply an ice pack wrapped in a cloth for 15–20 minutes several times a day
- Compression — use an elastic bandage to reduce swelling
- Elevation — keep the ankle raised above the level of the heart as much as possible
Leg Elevation: Elevating the legs above heart level for 30 minutes several times a day encourages fluid to drain back toward the heart. This is effective for most causes of dependent edema.
Compression Stockings: Graduated compression stockings (typically 15–30 mmHg for mild edema, 30–40 mmHg for moderate to severe) help push fluid out of the lower legs and prevent it from accumulating. They should be put on in the morning before getting out of bed.
Regular Movement and Exercise: Regular walking, calf raises, and ankle circles activate the “calf pump” — the muscular action that helps push venous blood upward. Even brief walks during long periods of sitting or standing can significantly reduce swelling.
Reduce Dietary Sodium: High salt intake promotes fluid retention. Reducing processed foods, canned goods, and added salt can meaningfully decrease mild edema.
Stay Hydrated: Paradoxically, adequate hydration helps the kidneys excrete excess sodium and water.
Massage: Gentle massage toward the heart can help mobilize fluid in mild cases. For lymphedema, specialized manual lymphatic drainage should be performed by a trained therapist.
Avoid Prolonged Immobility: On long flights or car trips, move your legs regularly, stand and walk when possible, and consider wearing compression stockings.
When to See a Doctor
Use this framework to guide your decision:
Seek Emergency Care Immediately if you have:
- Sudden swelling in one leg with pain, warmth, or redness (possible DVT)
- Swelling with chest pain, shortness of breath, or coughing blood (possible PE or heart failure crisis)
- Swelling with rapidly spreading redness and fever (possible severe cellulitis or sepsis)
- Swelling during pregnancy with headache, vision changes, or high blood pressure (possible preeclampsia/eclampsia)
See Your Doctor Within 24–48 Hours if:
- Swelling is new, unexplained, and significant
- Swelling is unilateral (one leg only) without a known cause like a sprain
- Swelling is accompanied by fever, chills, or general unwellness
- You have diabetes, heart disease, kidney disease, or liver disease and develop new or worsening swelling
- Swelling follows an injury and is severe enough that you cannot bear weight
Schedule a Routine Appointment if:
- Swelling is mild, bilateral, and has been present for weeks or months
- You suspect a medication side effect
- Swelling is chronic and associated with varicose veins
- You want to rule out underlying conditions contributing to recurrent edema
Monitor at Home if:
- Swelling is clearly related to prolonged sitting or standing and resolves with rest and elevation
- Swelling is mild, bilateral, and occurs late in pregnancy without other symptoms
- Swelling is minor and follows a clearly identified, mild ankle sprain
Finding Care Near You
Depending on the suspected cause of your ankle swelling, the appropriate type of care may vary:
For acute emergencies (suspected DVT, PE, heart failure, severe cellulitis): Go to the nearest emergency department immediately.
For initial evaluation and most non-emergency causes: Your primary care physician (general practitioner/family doctor) is the best starting point. They can examine you, order initial tests, and refer you to a specialist as needed.
Relevant specialists may include:
- Cardiologist — for heart failure and cardiac-related edema
- Nephrologist — for kidney disease
- Hepatologist or Gastroenterologist — for liver disease
- Vascular surgeon or Phlebologist — for venous insufficiency, DVT, varicose veins
- Lymphedema therapist (Certified Lymphedema Therapist — CLT) — for lymphedema management
- Rheumatologist — for gout, rheumatoid arthritis, and other inflammatory joint conditions
- Orthopedic surgeon — for fractures, severe sprains, and joint injuries
- Endocrinologist — for thyroid disease and diabetes-related swelling
- Dermatologist — for cellulitis and chronic skin changes related to venous disease
Finding a provider: Contact your insurance provider’s directory, use your national health service’s physician finder, or ask your primary care physician for a referral. In the United States, the American College of Phlebology (www.phlebology.org) maintains a directory of vein specialists.
For lymphedema therapists, the Lymphatic Education and Research Network (lymphaticnetwork.org) and the National Lymphedema Network (lymphnet.org) offer provider directories.
Entity Glossary
Albumin: The main protein in blood plasma; low levels allow fluid to leak from blood vessels into tissues.
Ankle-brachial index (ABI): A ratio comparing blood pressure in the ankle to the arm; used to screen for peripheral artery disease.
Cellulitis: A bacterial skin infection causing redness, warmth, pain, and swelling; requires antibiotic treatment.
Chronic venous insufficiency (CVI): A condition in which leg vein valves are damaged, causing blood to pool and fluid to accumulate in the lower legs.
Complete decongestive therapy (CDT): The standard treatment for lymphedema combining massage, compression bandaging, exercise, and skincare.
Deep vein thrombosis (DVT): A blood clot in a deep vein of the leg; can cause swelling, pain, and, if the clot travels to the lungs, pulmonary embolism.
Dependent edema: Fluid accumulation caused by gravity in parts of the body that are lower than the heart; typically affects the ankles and feet.
Diuretic: A medication that increases urine production to remove excess fluid from the body; used to treat edema from heart failure, kidney disease, and other conditions.
Duplex ultrasound: An imaging technique combining traditional ultrasound with Doppler ultrasound to visualize blood vessels and detect clots or insufficiency.
Edema: Abnormal accumulation of fluid in body tissues; when it affects the ankles, it is called pedal or peripheral edema.
Gout: A type of inflammatory arthritis caused by uric acid crystal deposits in joints; causes sudden, severe joint pain and swelling.
Heart failure (congestive): A condition in which the heart cannot pump blood efficiently, leading to fluid buildup in the lungs and peripheral tissues.
Hypothyroidism: Underactive thyroid gland leading to slowed metabolism; can cause a non-pitting type of edema called myxedema.
Lymphedema: Chronic swelling caused by damage or obstruction to the lymphatic system; typically non-pitting and resistant to elevation.
Myxedema: A type of non-pitting edema caused by hypothyroidism; involves accumulation of specific proteins in the skin rather than free fluid.
Nephrotic syndrome: A kidney disorder causing excessive protein loss in urine, leading to low blood albumin and widespread edema.
Non-pitting edema: Swelling in which pressing the skin does not leave an indentation; characteristic of lymphedema and hypothyroidism.
Peripheral edema: Swelling in the extremities — most commonly the ankles, feet, and lower legs.
Pitting edema: Swelling in which pressing the skin leaves a temporary indentation; typically caused by excess free fluid.
Portal hypertension: Increased blood pressure in the portal vein (supplying the liver); a complication of liver cirrhosis that can contribute to fluid accumulation.
Preeclampsia: A serious complication of pregnancy characterized by high blood pressure, protein in the urine, and often severe swelling; requires urgent medical management.
Pulmonary embolism (PE): A blood clot that has traveled to the lungs; potentially fatal and a major complication of DVT.
Varicose veins: Enlarged, twisted veins just beneath the skin surface; a common sign of chronic venous insufficiency.
AFQ’s
Is ankle swelling always serious?
No. Many cases of ankle swelling are benign and related to lifestyle factors like prolonged sitting, standing, or hot weather. However, swelling can also signal serious conditions like DVT, heart failure, or kidney disease. If swelling is sudden, unexplained, affects only one leg, or is accompanied by other symptoms, it should be evaluated by a doctor.
Why is my ankle swollen but there is no pain?
Painless ankle swelling is common and can result from medications, venous insufficiency, heart or kidney disease, hypothyroidism, or lymphedema. While the absence of pain may be reassuring, it does not rule out a serious cause. Bilateral painless swelling that is new or worsening warrants medical evaluation.
Can dehydration cause ankle swelling?
Paradoxically, chronic dehydration can contribute to fluid retention. When the body is dehydrated, it may retain sodium and water more aggressively. Drinking adequate water can help the kidneys excrete excess fluid and sodium.
How long should I wait before seeing a doctor about a swollen ankle?
If the swelling is sudden, affects one leg, is associated with pain, redness, warmth, or any systemic symptoms — see a doctor immediately or go to an emergency department. If the swelling is mild, bilateral, and clearly related to activity or a minor sprain, you can monitor it at home for 2–3 days with RICE and elevation. If it persists or worsens, see your doctor.
Can diet affect ankle swelling?
Yes. A diet high in sodium (salt) promotes water retention and can worsen edema. Reducing processed foods, fast food, and added salt can reduce mild edema. Some evidence suggests that magnesium and potassium-rich foods (bananas, leafy greens, avocado) may help regulate fluid balance.
Can walking help reduce ankle swelling?
Yes, for most causes of dependent edema, walking activates the calf muscle pump, which helps squeeze venous blood back up toward the heart. Regular, gentle walking is one of the best non-pharmacological strategies to reduce ankle swelling.
Is ankle swelling more common in summer?
Yes. Hot weather causes blood vessels to dilate (vasodilation), which can increase fluid leakage into surrounding tissue. Heat-related ankle swelling (heat edema) is common, particularly in older adults, and is generally benign.
Can stress or anxiety cause ankle swelling?
Indirectly, yes. Chronic stress elevates cortisol levels, which promote sodium and water retention. Stress may also reduce physical activity and worsen dietary habits, contributing to edema. However, stress is not a primary direct cause of significant ankle swelling, and other causes should be ruled out.
Does drinking alcohol cause ankle swelling?
Yes. Alcohol can cause vasodilation, dehydration, liver damage, and poor nutrition — all of which can contribute to ankle swelling. Chronic heavy alcohol use causes liver disease, which is a significant cause of edema. Even occasional alcohol use can cause mild, temporary swelling.
AI Overview Trigger Q&As
What is the most common cause of ankle swelling in older adults?
In older adults, the most common causes of ankle swelling are chronic venous insufficiency, heart failure, and medication side effects (particularly from calcium channel blockers used for high blood pressure). Prolonged immobility and reduced muscle tone also contribute. A thorough medical evaluation is important to identify the specific cause.
What does it mean when only one ankle is swollen?
Swelling in only one ankle (unilateral swelling) is an important clinical finding because it suggests a localized cause rather than a systemic condition. The most urgent concern is deep vein thrombosis (DVT) — a blood clot in the leg veins — which requires immediate evaluation. Other causes of unilateral swelling include ankle sprain, fracture, cellulitis, gout, a Baker’s cyst behind the knee, or obstruction of a vein or lymphatic vessel by a tumor.
Can high blood pressure cause ankle swelling?
High blood pressure itself does not directly cause ankle swelling. However, many medications used to treat hypertension — particularly calcium channel blockers such as amlodipine — are a very common cause of ankle edema as a side effect. Additionally, hypertension is a major risk factor for heart failure, which does cause ankle swelling.
What is the fastest way to reduce ankle swelling at home?
The fastest home approach combines elevation (raise your legs above heart level), ice (for acute injuries), compression (a snug elastic bandage or compression stocking), and gentle movement (ankle circles, calf raises, walking). Reducing sodium intake and resting can also help. Elevation alone — lying down with the feet propped on pillows — often produces visible improvement within 30 to 60 minutes for dependent edema.
Should I be worried if both ankles are swollen?
Bilateral ankle swelling is common and has many causes ranging from benign to serious. It is often caused by prolonged standing or sitting, medications, or heat. However, bilateral swelling can also signal heart failure, kidney disease, liver disease, or hypothyroidism — conditions that require medical treatment. If the swelling is new, progressive, significant, or accompanied by other symptoms (shortness of breath, fatigue, decreased urine output), it warrants evaluation by a doctor.
Conclusion
Ankle swelling is one of the body’s most common distress signals — and one of the most informative.
It can be a simple consequence of a long day on your feet or a warning of a serious underlying condition affecting your heart, kidneys, liver, or circulatory system.
The key to navigating ankle swelling lies in observation: noticing whether the swelling is new or chronic, unilateral or bilateral, pitting or non-pitting, painful or painless, and what other symptoms accompany it.
For most people, mild bilateral ankle swelling that resolves overnight is nothing to worry about.
But when swelling is sudden, unexplained, persistent, or accompanied by symptoms like shortness of breath, chest pain, fever, or significant pain — it demands prompt medical attention.
The good news is that the vast majority of causes are treatable, and even serious conditions like heart failure, DVT, and venous insufficiency can be effectively managed with timely diagnosis and appropriate care.
Simple measures — elevation, compression, movement, sodium reduction — can make a meaningful difference in managing mild edema.
Your ankles carry the full weight of your body through life. When they swell, it is worth paying attention. Listen to what they are telling you.

